by: Jennifer Oldfield
The month of March is Poison Prevention Awareness Month and we have had 2 posts this month on toxins to your pet, but sometimes things that aren’t technically toxic can be just as problematic if swallowed. Occasionally cats, but much more frequently dogs, will eat items that really aren’t intended to be edible; items such as rocks, all kinds of toys, socks, even gloves. In many cases if the item is small they are able to pass them through their system, or they will vomit them up, but sometimes they end up caught part way through being digested and surgery becomes required to remove the item.
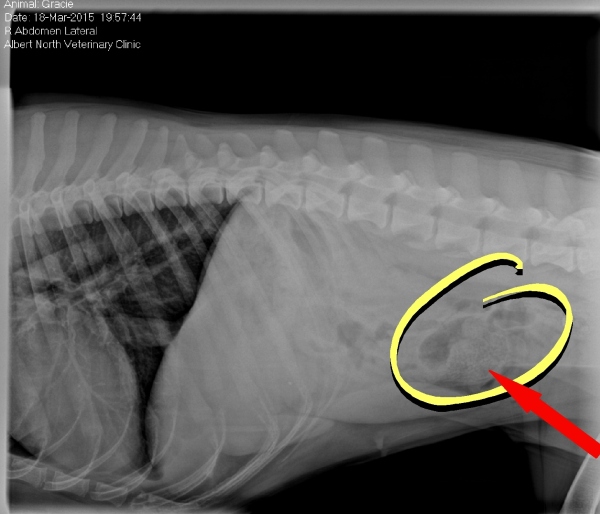
Grace is one such dog who required surgery. Her story is fairly simple. One day she threw-up a gardening glove. Grace appeared fine but her owner exercised caution and gave her a very small meal. She didn’t vomit again, so a bit later she gave her more food. She ended up vomiting all of it up. Without hesitation Grace was brought in to us. Although Dr. Liebe could feel a foreign body in Grace’s abdomen x-rays were taken to confirm.
Dr. Liebe got Grace into surgery right away. The surgery only lasted 30 mins. She was able to remove the foreign body (which turned out to be the other glove) and sew her back up without requiring any additional surgery time, thanks to Grace’s owner acting quickly and bringing her in right away.
Why is that time so important? What difference would 12 or 24 hours have made?
There are 2 answers to that question:
- Especially quickly in cats, but certainly also in dogs, they can become sick enough that they don’t make it
- Provided surgery can occur it is higher risk due to;
- possible dehydration
- abnormal blood results because the body is trying to fight what it sees as an infection
- the tissue surrounding the foreign body begins to die (labelled in the image below as hypoxic intestine)
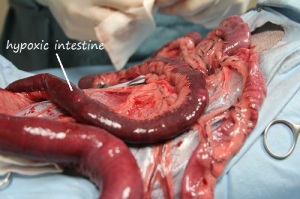 Often the surgery to remove a foreign body is an hour or more in length. This is due to the necessity of removing a section of the intestines, anywhere from a few inches to, on rare occasion, as much as a foot.
Often the surgery to remove a foreign body is an hour or more in length. This is due to the necessity of removing a section of the intestines, anywhere from a few inches to, on rare occasion, as much as a foot.
For your pet to have the best case scenario the sooner you get them in the better. Our basic rule of thumb is:
- if you know they have eaten something they shouldn’t have, but you think they can pass it, monitor them
- if they are having diarrhea or vomiting they should be seen as soon as possible
- if they can’t keep anything down (especially water) do NOT wait any longer, they need to be seen immediately.
Ideally we will see your pet prior to getting to #3. If your pet ate something and you are unsure if it will pass, please always call your veterinarian, they are your best source for information.
To see a video clip of part of Grace’s surgery, click here.








 However, more and more items are containing this lethal toxin – chewable vitamins, dental hygiene products, even some prescription medications. You can also purchase a bag of xylitol to use as a sugar substitute at home.
However, more and more items are containing this lethal toxin – chewable vitamins, dental hygiene products, even some prescription medications. You can also purchase a bag of xylitol to use as a sugar substitute at home. “The cause of xylitol-related liver failure in dogs is not well understood, but scientists suspect it has to do with the fact that xylitol and its metabolites deplete adenosine triphosphate stores in the liver. Adenosine triphosphate is a chemical substance that gives cells energy. Without a sufficient amount of this chemical, the cells in the liver die off”.*
“The cause of xylitol-related liver failure in dogs is not well understood, but scientists suspect it has to do with the fact that xylitol and its metabolites deplete adenosine triphosphate stores in the liver. Adenosine triphosphate is a chemical substance that gives cells energy. Without a sufficient amount of this chemical, the cells in the liver die off”.*
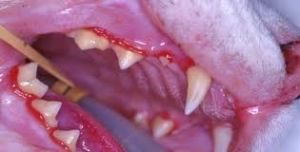 Teeth are held in place by the bones, ligaments, and gums surrounding them. Periodontal disease is the progressive loss or destruction of these tissues around the teeth, and can lead to infection and loss of teeth. The earliest sign of periodontal disease is gingivitis. This is inflammation of the gums caused by the body’s inflammatory response to plaque. Plaque is the biofilm of bacteria and their by-products, salivary components, and oral debris that accumulate on the teeth. It is what is removed during brushing. If not brushed off, plaque mineralizes to form tartar/calculus within about 24 – 48 hours, and this promotes the accumulation of even more plaque. Brushing does not get rid of tartar; it can only be removed by scaling. Gingivitis can be reversed with a proper dental cleaning. Just remember, if the gums are red, they are infected and painful!
Teeth are held in place by the bones, ligaments, and gums surrounding them. Periodontal disease is the progressive loss or destruction of these tissues around the teeth, and can lead to infection and loss of teeth. The earliest sign of periodontal disease is gingivitis. This is inflammation of the gums caused by the body’s inflammatory response to plaque. Plaque is the biofilm of bacteria and their by-products, salivary components, and oral debris that accumulate on the teeth. It is what is removed during brushing. If not brushed off, plaque mineralizes to form tartar/calculus within about 24 – 48 hours, and this promotes the accumulation of even more plaque. Brushing does not get rid of tartar; it can only be removed by scaling. Gingivitis can be reversed with a proper dental cleaning. Just remember, if the gums are red, they are infected and painful!
